ICRS 2019 - Conference Calendar
16.3.1 - Distinctive long-term migration of adipogenic niche in the rabbit: biological perspectives for osteoarthritis clinical headway
- G. Desando (Bologna, IT)
- I. Bartolotti (Bologna, IT)
- L. Martini (Bologna, IT)
- N. Nicoli Aldini (Bologna, IT)
- G. Giavaresi (Bologna, IT)
- M. Fini (Bologna, IT)
- A. Roffi (bologna, IT)
- E. Kon (Milano, IT)
- F. Perdisa (Ozzano Dell'Emilia (BO), IT)
- G. Filardo (Bologna, IT)
- B. Grigolo (Bologna, IT)
- L. Andriolo (Bologna, IT)
Abstract
Purpose
The understanding of cell migration after cell-based treatments is growing in osteoarthritis (OA), as it might influence the clinical outcome. Among biological alternatives, the adipose “niche” is emerging as a promising therapy being a rich cell source which can be available by enzymatic (SVF) and mechanical (MFAT) techniques. Herein, we investigated the migratory profile of expanded-adipose stromal cells (ASCs), SVF, and MFAT in a rabbit OA model at 7 and 30 days follow-up.
Methods and Materials
A mild grade of OA was surgically induced by bilateral anterior cruciate ligament transection in 18 rabbits. ASCs (n=6) and SVF (n=6) were obtained by collagenase NB4 treatment, whereas MFAT (n=6) by the mechanical technique in a one-step closed system (Lipogems device). In vitro biological studies on cells viability, surface marker characterization and morphology were carried out. For local biodistribution analysis, cells were labeled with PKH26, a fluorescent lipophilic membrane binding dye. After OA onset, 2x106 ASCs, SVF, and MFAT were intra-articularly injected into the knee joint and local biodistribution was evaluated at 7 and 30 days. Assessments on cell biodistribution and colocalization for PKH26 and CD-146 were done at short and long-term follow-ups. Histological assessments supported by specific scoring systems on osteochondral tissues and synovial membrane were carried out. The Monte Carlo method and the general linear model for multiple comparisons were used for statistics.
Results
High cell viability and a distinct long-term migration were noticed for all groups. At day 7, ASCs and SVF displayed a high tropism for synovium while MFAT for cartilage; an opposite trend was noticed at day 30. Cartilage repair was noticed after MFAT, likewise to ASCs treatment.
Conclusion
The long-term presence of adipose cells might have a clinical significance ensuring a cellular reservoir to promote repair processes. The different migration could open interesting clinical insights on their use for OA treatment.
16.3.2 - Syndecan-4 is Increased in Osteoarthritic Knee, but not Hip or Shoulder, Articular Hypertrophic Chondrocytes
Abstract
Purpose
Syndecans are transmembrane heparan sulfate proteoglycans that regulates cell-matrix interactions. Though their glycosaminoglycan chains, syndecans interact with a variety of extracellular matrix molecules as well as with growth factors and cytokines. They are involved especially in embryonic development, tumorigenesis, and angiogenesis Syndecans are expressed by chondrocytes] but their role in cartilage homeostasis or degradation remain poorly documented. We suspect that syndecan-4 plays a critical role in cartilage degradation during osteoarthritis (OA).The aim of this study was to investigate the expression and localization of syndecan-4 in different OA joint tissues.
Methods and Materials
Syndecan-4 mRNA levels were quantified by RT-PCR in human OA primary cells. Syndecan-4 was localized by immunohistochemistry in knee, hip or shoulder OA bone/cartilage biopsies. Syndecan-4 was quantified by immmunoassay in chondrocytes culture supernatant and cell fraction.
Results
Using immunochemistry, syndecan-4 was observed in chondrocytes clusters in the superficial zone of OA knee, but not in OA hip or shoulder cartilage. No significant difference was detected in syndecan-4 expression level in sclerotic compared to non-sclerotic osteoblasts or in inflamed synoviocytes compared to normal/reactive ones. Differentiated hypertrophic chondrocytes from knee, but not from hip cartilage, expressed more syndecan-4 than non-hypertrophic cells. Using an immunoassay for the extracellular domain of syndecan-4, we found 68% of the syndecan-4 in the culture supernatant of OA chondrocytes culture, suggesting that a large majority of the syndecan-4 is shed and released in the extracellular medium. The shedding rate was not affected by hypertrophic differentiation state of the chondrocytes or their joint origin.
Conclusion
Even if chondrocytes clusters are seen in OA knee, hip and shoulder cartilage and hypertrophic differentiation appears in knee and hip OA articular chondrocytes, syndecan-4 synthesis only increased in knee. These findings suggests the presence of biochemical difference between articular cartilage according to their location and that syndecan-4 could be a biochemical marker specific for knee OA.
16.3.3 - Long term efficacy of Micro-fragmented adipose tissue in the treatment of Knee Osteoarthritis
Abstract
Purpose
Intra-articular injection of Micro-fragmented adipose tissue (MAT) is a minimally invasive technique that has shown promising results for improving function and reducing pain in patients suffering with arthritis. Current treatments, including joint replacement, carry huge risk and if performed in those under the age of 55 can produce poorer outcomes and require revision surgery. The aim of the study was to evaluate the clinical outcomes of patients with knee osteoarthritis (KOA), 1-year following MAT treatment.
Methods and Materials
Pre-op
Patients with KOA were x-rayed to assess severity and scored using VAS and OKS. All patients with measures of VAS ≥5 and OKS <30 were included in the study (n=96 with n=43 at 1 year).
Procedure
Autologous adipose tissue was aspirated from each patient under sedation administered by an anaesthetist, and micro-fragmented using the Lipogems system. The MAT was then injected, using ultrasound guidance, into the affected joint.
Post-op
At 3, 6 and 12 months, patients VAS and OKS measures were rescored and evaluated.
Results
A significant change was recorded comparing pre- and post-operative outcome measures. VAS scores saw improvement (p<0.001) from a mean value of 6.90±1.49, at 3 (3.49±2.65), 6 (3.77±2.86), and 12 months (3.52±3.09). OKS saw improvement (p<0.001) from a mean value of 21.31±5.59, at 3 (31.18±9.41), 6 (29.90±10.31), and 12 months (30.93±8.16). Positive responses for VAS and OKS were observed for >80% of patients at 3, 6, and 12-month follow-ups.
Conclusion
The study demonstrates a significant improvement 1-year following MAT treatment for patients suffering KOA. Most patients experienced reduced pain and increased functionality. Paired with the minimally invasive approach, MAT looks to be an ideal interim treatment for joint arthritis that can delay the need for arthroplasty, preserving the native joint and delaying replacement. Further studies are required to identify the point at which efficacy may be lost.
16.3.4 - Machine learning predicts rate of cartilage loss: data from the Osteoarthritis Initiative
Abstract
Purpose
The rate of cartilage loss can vary widely between patients at risk or suffering from knee osteoarthritis (OA) but its causes remain unknown. We investigate whether quantitative and semi-quantitative radiographic features can be used to predict the rate of Joint Space Width (JSW) loss.
Methods and Materials
We collected bilateral knee radiographs, obtained by the OAI study, from 4100 patients (2383 female, 1717 male). Each patient was imaged up to 7 times, separated by at least 12 months, across a time span of 8 years. Each radiograph was analyzed by software to obtain Kellgren-Lawrence (KL) and OARSI grades for Osteophytes, Sclerosis and Joint Space Narrowing (JSN) readings, as well as JSW measurements for each individual knee. Individual knees with rate of JSW loss above 0.072 mm/year (the average yearly loss within JSN grade) were classified as progressors (956 knees). From these, knees in the top 10% of JSW loss rate were classified as fast progressors (91 knees). A logistic regression model was used to predict the fast progressor phenotype with KL and OARSI grades at baseline as independent variables. Model performance was estimated using 10-fold cross-validation dataset splits and used Area Under the Curve (AUC) as performance criteria.
Results
The logistic regression classifiers achieved AUCs of 0.71 (SE 0.015) and 0.66 (SE 0.013) at classifying individual knees as fast progressors for medial and lateral compartments, respectively. Analysis of the individual coefficients of the classifiers reveals that JSN and Sclerosis grades are the main predictors of rapid cartilage loss.
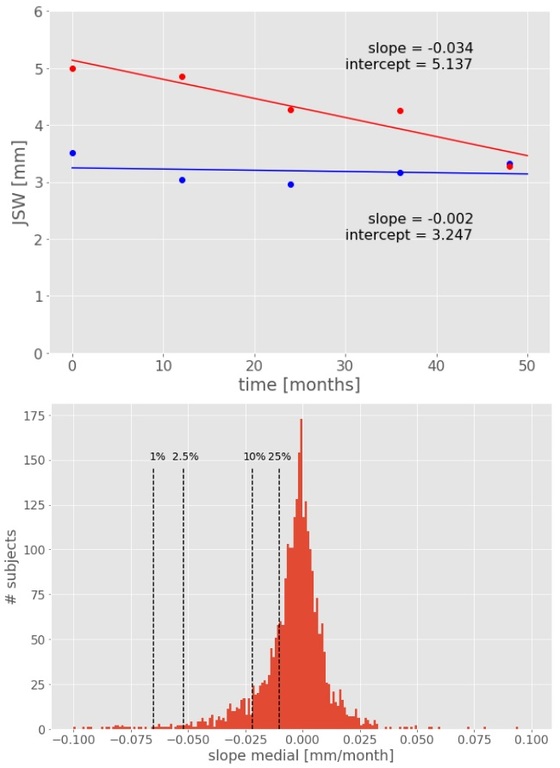
Conclusion
Our results show that it is possible to predict future rapid cartilage loss from readings from a single plain radiograph. Interestingly, neither KL grade nor Osteophytes OARSI grade contributed greatly to this prediction. Instead, Sclerosis and JSN grade seem to be the major predictors of rapid cartilage loss, suggesting a non-canonical mode of OA progression.
16.3.5 - Platelet-rich Plasma for the Treatment of Sport-active Patients with Knee Osteoarthritis: Limited Return to Sport.
Abstract
Purpose
In the last years, platelet-rich plasma (PRP) has been proposed for the treatment of knee osteoarthritis and its use is now supported by increasing evidences. Although recent reviews and meta-analysis showed good results using PRP for the treatment of knee osteoarthritis, the literature is still sparse on the use of PRP for the treatment of active patients. Aim of this study is to evaluate a cohort of sport-active patients suffering from cartilage degeneration and OA, in terms of clinical outcome and return to sport (RTS) after PRP injective treatment.
Methods and Materials
The study included forty-seven sport-active patients ≤50 years old with unilateral symptomatic knee cartilage degeneration or osteoa. Patients received 3 PRP injections and were prospectively evaluated at baseline and then at 2, 6, 12, and 24 months follow-up by IKDC subjective EQ-VAS, and Tegner scores. Furthermore, patients were asked about their return to sport, both in terms of return to any sport level or to their activity level before symptoms onset.
Results
IKDC subjective score improved significantly at all follow-ups, changing from 59.2±13.6 to 70.6±13 at 12 months and 76.7±12.5 at 24 months. A similar outcome was observed with the EQ-VAS score. Tegner score improved from 3.6±1.4 to 4.8±0.9 at 24 months, but only 76.6% of patients returned to some kind of sport activity and 48.9% to the same activity level. A lower pre-symptoms Tegner score was associated with a higher return to sport rate, both at any level and at the same level.
Conclusion
Sport-active patients affected by knee osteoarthritis can benefit from PRP injections, with pain and function improvement. However, results are less satisfactory in terms of return to sport since only half can achieve the same sport level as before the onset of symptoms. Patients undergoing PRP treatment should be aware of their low chances to go back to high-impact sport activities.
16.3.6 - Rescue Injection of Amniotic Suspension Allograft Improves Pain and Function in Patients with Knee Osteoarthritis
Abstract
Purpose
Osteoarthritis (OA) affects 30.8 million Americans; over 54% of these patients are estimated to require joint replacement during their lifetime. A multi-center randomized trial was conducted to investigate the effects of amniotic suspension allograft (ASA) in comparison to saline and hyaluronic acid (HA). Within this study there was an option for rescue if there was inadequate pain relief with the index injection. The purpose of the current study was to examine the effects of rescue injections compared to the patient’s initial treatment.
Methods and Materials
200 patients from 12 sites were randomized 1:1:1 to either saline, HA, or ASA. Patients (blinded) received a single intra-articular injection and were followed for 12 months. At 3 months, patients who self-reported unacceptable pain were eligible to receive ASA (if their initial randomization was saline or HA). ASA patients who reported unacceptable pain were offered standard of care management (outside of the study). Rescued patients (n=94) were followed from rescue (new baseline) to 12 months post-rescue. Changes from baseline to 3 months follow-up (original) were compared to changes from rescue baseline to the 3-month rescue visit using Knee Injury and Osteoarthritis Outcome Score (KOOS) and Visual Analog Scale (VAS). Statistical comparisons were made using LSMEANS with p-values from PROC MIXED.
Results
Patients who were rescued with ASA had significantly greater improvements in KOOS pain scores (original Δ 4.62, rescue Δ 12.29; p=0.0044) and ADL scores (original Δ 5.55, rescue Δ 10.94; p=0.0432) compared to their original treatment course (saline or HA). Furthermore, rescued patients had significantly greater improvements in VAS pain with a rescue injection (original Δ -9.44, rescue Δ -27.26; p=0.0064).
Conclusion
Patients who received a rescue injection of ASA showed significantly greater improvements compared to their initial treatment. This data provides evidence for the potential use of ASA in the treatment of knee OA symptoms.
16.3.7 - Surface modification on biomaterials with synovium-derived mesenchymal stem cells-affinity peptide for tissue engineering
Abstract
Purpose
Synovium-derived mesenchymal stem cells (SMSC) have been studied for over a decade since first being successfully isolated in 2001. These cells demonstrate the most promising therapeutic efficacy for musculoskeletal regeneration of the MSC family, particularly for cartilage regeneration. However, the mobilization and transfer of MSCs to defective or damaged tissues and organs in vivo with high accuracy and efficiency has been a major problem in tissue engineering (TE).Methods and Materials
In the present study, we identified a seven amino acid peptide sequence [SMSCs-affinity peptide (LTHPRWP; L7)] through phage display technology that has a high specific affinity to SMSCs. Thereafter, L7 was covalently conjugated onto both polycaprolactone (PCL) electrospun meshes and human decalcified bone scaffolds (hDBSc) to investigate its TE applications.Results
Our analysis suggested that L7 efficiently and specifically interacted with SMSCs without any species specificity. After 24 h coculture with human SMSCs (hSMSCs), L7-conjugated PCL electrospun meshes had significantly more adherent hSMSCs than the control group, and the cells expanded well. Similar results were obtained using hDBSs. These results suggest that the novel L7 peptide sequence has a high specific affinity to SMSCs. Covalently conjugating this peptide to either artificial polymer material (PCL mesh) or natural material (hDBS) significantly enhances the adhesion of SMSCs.Conclusion
This method is applicable to a wide range of potential SMSC-based TE applications, particularly to cartilage regeneration, via surface modification on various type of materials.16.3.8 - A novel quantitative metric for joint space width: data from the Osteoarthritis Initiative
Abstract
Purpose
Joint Space Width (JSW) has been the gold standard to assess loss of cartilage in knee OA. Here we describe a novel quantitative measure of joint space width, standardized JSW (stdJSW). We assess the performance of this quantitative metric for joint space widthat tracking Joint Space Narrowing OARSI grade (JSN) changes and provide reference values for different joint space narrowing OARSI grades and their annual change.
Methods and Materials
We collected 18.934 individual knee images from the OAI study, from the follow-up visits up to month 48 (baseline plus 4 follow-up exams). Absolute JSW measurements and JSN readings were collected from the OAI study. Standardized JSW and 12-month changes were calculated for each knee. For each JSN grade and 12-month grade change, the distribution of JSW loss was calculated both for standardized JSW as well as absolute JSW measurements retrieved from the OAI study. Area under the curve of the ROC curves was calculated for the performance of both absolute and standardized JSW at discriminating between different JSN grades. Standardized response mean (SRM) was used to compare the responsiveness of the two measures to change in JSN grade.
Results
The areas under the ROC curve for stdJSW at discriminating between successive JSN grades were AUCstdJSW= 0.87, 0.95, and 0.96, for JSN>0, JSN>1 and JSN>2, respectively, whereas these were AUCfJSW= 0.79, 0.90, 0.98 for absolute JSW. We find that standardized JSW is significantly more responsive than absolute JSW, as measured by the Standardized Response Mean. Furthermore, we present reference values for standardized JSW stratified by base JSN grade and 12-month JSN change.
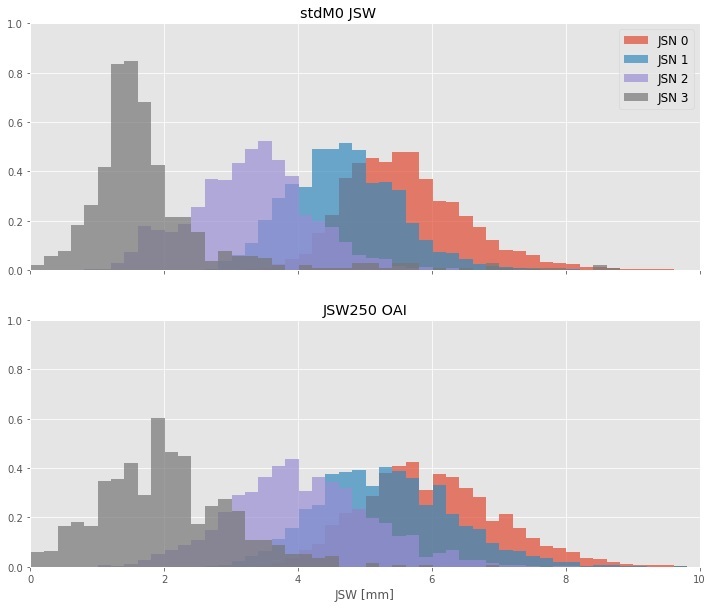
Conclusion
Our results show that standardized JSW is a better choice to track changes in JSN and to discriminate between JSN grades. Furthermore, our results show that standardized JSW cancels part of the normal variation in JSWs that comes from height variation.
16.3.9 - Vitamin D3 inhibits ADAMTS-4 and MMP13
Abstract
Purpose
OA develops because it is an imbalance between catabolic and anabolic processes resulting in gradual degradation of cartilage. Inflammation and mechanical strain are the causes of increased degradation. It is therefore of utmost importance to find a drug or a natural molecular substance that can stop catabolic processes. Several studies have suggested a link between vitaminD status and OA; some have found that individuals deficient in vitaminD have an increased risk of progressive knee-osteoarthritis, and there are reports of a pain reducing effect of oral supplementation. Of importance, vitaminD has been suggested to dampen inflammation-driven diseases such as OA. VitaminD has been detected in the synovial fluid and chondrocytes express the vitaminD receptor. The aim of this study was to investigate if the vitaminD affects the expression of some of the regulatory proteins that regulate cartilage catabolism, focusing on the metabolism of Aggrecan and Collagen2.
Methods and Materials
Cells, taken from patients with secondary OA, were cultured in monolayer and treated with vitaminD. Half of the cells were also treated with IL1B to mimic an inflammatory condition. The expression of GDF5, ADAMTS-4 and MMP-13 were analyzed with qPCR. The cell medium was collected and ELISA was performed to quantify the amount of the Aggrecan neoepitope ARGS, generated from ADAMTS-4-mediated cleavage of Aggrecan.
Results
VitaminD downregulated the expression of ADAMTS-4, MMP-13, both in the absence and presence of IL1β. IL1β itself had a significant stimulating effect on the expression of these genes. Furthermore, vitaminD upregulated the expression of TIMPs, as well as GDF5, a protein known to stimulate anabolic processes. Quantification of neoepitopes of Aggrecan is still performed.
Conclusion
VitaminD prevents degradation of Collagen and Aggrecan by downregulating the Aggrecan-specific proteinase ADAMTS-4 and Collagen-specific proteinase MMP-13 and also, by upregulating TIMP-1, TIMP-2 and TIMP-3, inhibitors of ADAMTs and MMPs.
16.3.10 - Comparison of Two Different Cartilage Repair Procedures with Concomitant High Tibial Osteotomy for Varus Knee Osteoarthritis
Abstract
Purpose
Cell-based tissue engineering approaches that use mesenchymal stem cells (MSCs) have addressed the issue of articular cartilage repair in knee osteoarthritis (OA). However, the most effective method of cartilage repair procedures has not been established. This study aimed to compare the clinical, radiological, and second-look arthroscopic outcomes related to two different cartilage repair procedures (implantation of MSCs or MSCs with allogenic cartilage) with concomitant high tibial osteotomy (HTO).
Methods and Materials
: Seventy patients treated with cartilage repair procedures and concomitant HTO were prospectively randomized into 2 groups: MSC implantation (MSC group), and implantation of MSCs with allogenic cartilage (MSC-AC group). Clinical outcomes were evaluated using the Lysholm Score and the Knee Injury and Osteoarthritis Outcome Score. Radiological outcomes were evaluated by measuring the femorotibial angle and posterior tibial slope. During second-look arthroscopy, cartilage regeneration was evaluated according to the Kanamiya grade.
Results
Clinical outcomes at the second-look arthroscopy improved significantly in both groups (P < 0.001 for all). Further improvement of clinical outcomes from the second-look arthroplasty to the final follow-up was observed only in the MSC-AC group (P < 0.05 for all). Overall, the Kanamiya grades, which were significantly correlated with clinical outcomes, were significantly higher in the MSC-AC group than in the MSC group. Radiological outcomes at final follow-up revealed improved knee joint alignments relative to preoperative conditions, but there was no significant correlation between clinical outcomes and Kanamiya grade in either group (P > 0.05 for all).
Conclusion
Implantation of MSCs with allogenic cartilage is superior to implantation of MSCs alone in cartilage regeneration accompanied with better clinical outcomes.



