Presenter of 1 Presentation
GLOBAL HYPERPERFUSION IS ASSOCIATED WITH A WORSE OUTCOME AMONG ACUTE ISCHEMIC STROKE PATIENTS UNDERWENT SUCCESSFUL ENDOVASCULAR TREATMENT
Abstract
Background and Aims
Patients with stroke may sometimes develop hyperperfusion after successful endovascular treatment (EVT). It is yet to be elucidated which factors affect post-EVT hyperperfusion and how hyperperfusion is associated with clinical outcome.
Methods
Consecutive patients who underwent EVT for anterior circulation occlusion and achieved successful recanalization (modified treatment in cerebral ischemia 2b–3) were reviewed. Hyperperfusion was categorized as follows based on post-EVT arterial spin labeling MRI: global hyperperfusion, increased cerebral blood flow (CBF) in ≥50% of previously occluded territory; focal hyperperfusion, increased CBF in <50% of previously occluded territory; and no hyperperfusion, no visible CBF increase. Factors associated with hyperperfusion were assessed and clinical outcome was compared among the hyperperfusion categories.
Results
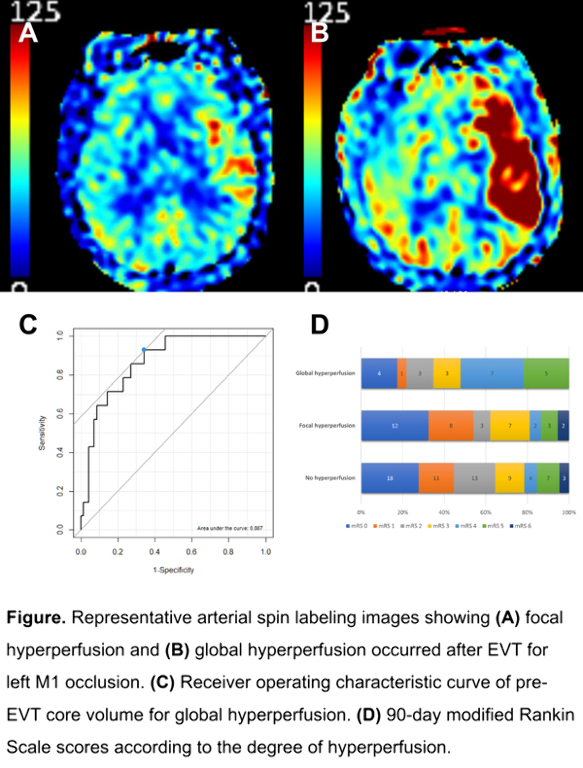
Among 125 eligible patients, 23 and 37 patients developed global and focal hyperperfusion, respectively. Compared with patients without hyperperfusion (n=65), global hyperperfusion group had worse neurologic severity and larger pre-EVT core. No significant difference was found between focal and no hyperperfusion groups. Pre-EVT core volume predicted global hyperperfusion with 92.9% sensitivity and 65.7% specificity (area under receiver operating characteristic curve, 0.867; 95% CI, 0.779–0.956). Global hyperperfusion group had worse 90-day outcome compared with focal hyperperfusion (modified Rankin Scale 0–2, 34.8% vs. 62.2%, p=0.072), and no hyperperfusion (34.8% vs. 64.6%, p=0.025) groups. Hemorrhagic transformation occurred similarly in the three groups.
Conclusions
Global hyperperfusion was associated with worse clinical outcome and tended to occur in patients with larger pre-EVT core. Future research is warranted to determine whether intervention such as blood pressure lowering improves outcomes in patients with global hyperperfusion.
