
Erik Koomen (Netherlands)
UMCU Wilhelmina Childrens Hospital Pediatrics, PICUAuthor Of 4 Presentations
BIG DATA IN PAEDIATRIC CARDIAC ARREST – TRICK OR TREAT?
TOWARDS A EUROPEAN NICU AND PICU DATA SHARING FRAMEWORK: AN ESPNIC INITIATIVE
Abstract
Background and Aims
A framework to safely share clinical data from European Pediatric and Neonatal Intensive Care Units (PICU, NICU) will enhance research, improve clinical benchmarking and promote quality improvement projects among participating centres. When applying advanced data science methods such as machine learning to heterogenous patient data, substantial amounts of patient data from different centres may be needed to produce and validate reliable models.
The aim of this research is to summarize conditions and requirements which such a framework must meet in order to take the first steps towards a European NICU and PICU clinical data framework.
Methods
A survey was conducted among the members of the ESPNIC Data Science Working Group to investigate the use of electronic medical records (EMR) among European NICU’s and PICU’s and to identify European experts in NICU and PICU data registries and data science. During three meetings, these experts defined a list of topics regarding the framework conditions and requirements.
Results
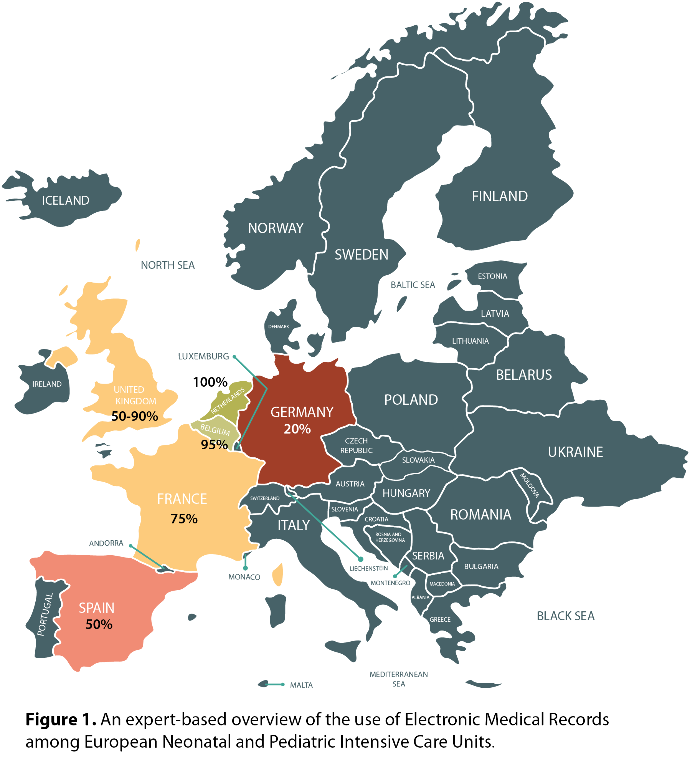
The use of EMR ranged from approximately 20% in Germany to 100% in The Netherlands (Figure 1). Fourteen European experts in data registries and data science were identified. They reached consensus on the requirements for a European NICU and PICU data framework, which included data availability, data standardization, legislation and privacy, funding and framework architecture.
Conclusions
Several requirements for a European NICU and PICU clinical data sharing framework were identified, including data availability. The variable use of EMR among European centres may detain development of such a framework.
PREDICTION OF PEWS AT PICU; THE USE OF A NEW MACHINE LEARNING METHOD
Abstract
Background and Aims
The increasing amounts of data pose a great demand on ICU staff because of data overload. Medical decision making is a difficult and labor-intensive process, especially with multiple, continuous streams of vital sign data. Machine learning (ML) may be used to support decision making by facilitating the recognition of clinical patterns in this data.
Methods
This single-center, retrospective, cohort study included 1208 patients admitted to the PICU of the University Medical Center Utrecht, The Netherlands. Six streams of recorded vital signs (Figure1) were collected from the EMR, resulting in a set of 1,5 million data time points. The ML method uses Symbolic Aggregate approXimation (SAX) to summarize the streams of vital signs leading up to and including the current time point. The patient of interest is then matched with historic patients based on those SAX patterns. The disease courses of the matched patients are aggregated into a predicted disease course for each vital sign. To get a summary of predictive performance across multiple variables, the vital signs are combined into a Pediatric Early Warning Score (PEWS).
Results
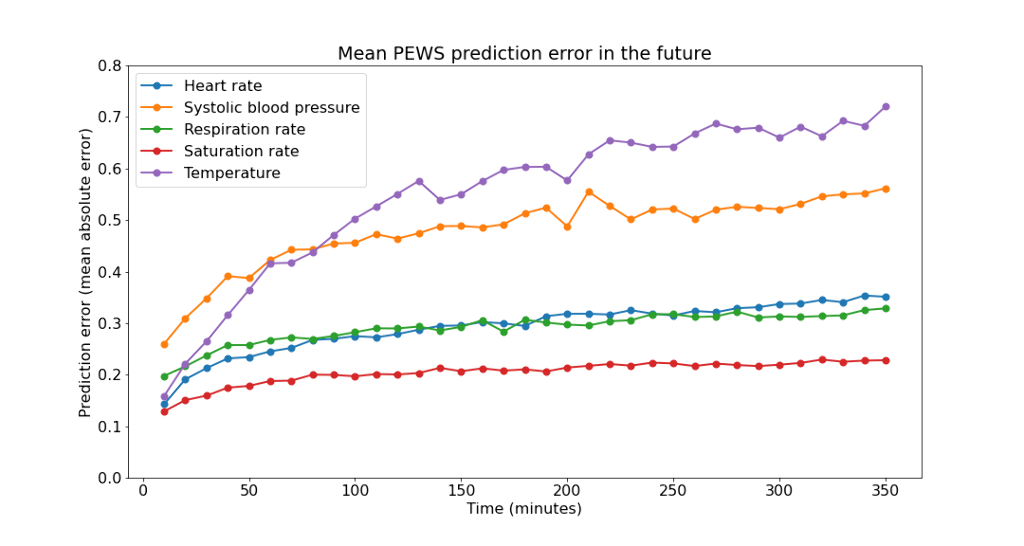
 Predictions of vital signs show reasonable errors, slightly increasing as time progresses (Figure1). The PEWS predictions are compared to the observed, calculated PEWS, showing reasonable calibration (Figure2).
Predictions of vital signs show reasonable errors, slightly increasing as time progresses (Figure1). The PEWS predictions are compared to the observed, calculated PEWS, showing reasonable calibration (Figure2).
Conclusions
Vital sign prediction at the PICU showed the first promising steps in the use of new Machine Learning strategies to optimize care.
MACHINE LEARNING ON PAEDIATRIC INTENSIVE CARE DATASETS TO IMPROVE MORTALITY PREDICTION MODELS
Abstract
Background and Aims
Paediatric intensive care unit (PICU) mortality prediction models, such as the Paediatric Index of Mortality (PIM) are historically based on manual data entry and retrieval. Presently, Electronic Medical Record (EMR) systems contain more detailed and/or more frequently measured data. The aim of this study was to assess whether machine learning (ML) on PICU datasets extracted from the EMR outperform existing mortality prediction models.
Methods
Data from patients admitted to the PICU of the University Medical Center Utrecht, The Netherlands, between 2009 and 2018 were collected. Variables from existing prediction models (PIM2, PIM3, Paediatric Risk of Mortality (PRISM) III) were extracted from the local Dutch PICU quality registry (PICE), whereas vital signs and laboratory values were extracted from a local PICU research data warehouse. Logistic regression, support vector machines and random forest were fitted on the dataset using hold-out validation. Variables were selected both manually as via algorithms. All existing and ML models were evaluated by comparing their areas under the receiver operating characteristics (AUROCs).
Results
PIM3 was the best performing existing mortality score with an AUROC of 88% [95%CI 81%-90%]. The AUROC’s of the different tested ML methods, pre-processing, and hyperparameter combinations fluctuated heavily (30%-90%). Logistic regression had superior performance with an AUROC 93.1% [95%CI 91%-95%] fitted on the PICE dataset in combination with laboratory values.
Conclusions
Interpretable ML models can improve existing prediction models on PICU mortality, with the addition of EMR data. Further improvement of the models with real time predictions could improve clinical application.
Presenter of 2 Presentations
BIG DATA IN PAEDIATRIC CARDIAC ARREST – TRICK OR TREAT?
PREDICTION OF PEWS AT PICU; THE USE OF A NEW MACHINE LEARNING METHOD
Abstract
Background and Aims
The increasing amounts of data pose a great demand on ICU staff because of data overload. Medical decision making is a difficult and labor-intensive process, especially with multiple, continuous streams of vital sign data. Machine learning (ML) may be used to support decision making by facilitating the recognition of clinical patterns in this data.
Methods
This single-center, retrospective, cohort study included 1208 patients admitted to the PICU of the University Medical Center Utrecht, The Netherlands. Six streams of recorded vital signs (Figure1) were collected from the EMR, resulting in a set of 1,5 million data time points. The ML method uses Symbolic Aggregate approXimation (SAX) to summarize the streams of vital signs leading up to and including the current time point. The patient of interest is then matched with historic patients based on those SAX patterns. The disease courses of the matched patients are aggregated into a predicted disease course for each vital sign. To get a summary of predictive performance across multiple variables, the vital signs are combined into a Pediatric Early Warning Score (PEWS).
Results

 Predictions of vital signs show reasonable errors, slightly increasing as time progresses (Figure1). The PEWS predictions are compared to the observed, calculated PEWS, showing reasonable calibration (Figure2).
Predictions of vital signs show reasonable errors, slightly increasing as time progresses (Figure1). The PEWS predictions are compared to the observed, calculated PEWS, showing reasonable calibration (Figure2).
Conclusions
Vital sign prediction at the PICU showed the first promising steps in the use of new Machine Learning strategies to optimize care.
