John P. Corbett, United States of America
University of Virginia Center for Diabetes TechnologyPresenter of 2 Presentations
UTILIZING BEHAVIORAL PROFILES IN A MULTISTAGE MPC TO IMPROVE POSTPRANDIAL GLUCOSE CONTROL
Abstract
Background and Aims
Postprandial glucose control is often difficult due to the time constants associated with insulin action. We aim to reduce postprandial hyperglycemia by creating an artificial pancreas (AP) framework that anticipates meals using patterns found from past eating behavior.
Methods
Oral glucose appearance profiles were created using daily meal records (75% training, 25% testing) from a subject that exhibits well-defined eating patterns (breakfast, lunch, and dinner). The novel AP is a hybrid multistage model predictive control (MS-MPC) that treats meal profiles as glucose subsystem disturbances. Simulations using testing data were performed for all 100 adult subjects in the UVA/Padova simulator. MS-MPC results were compared to a hybrid MPC not informed by meal profiles.
Results
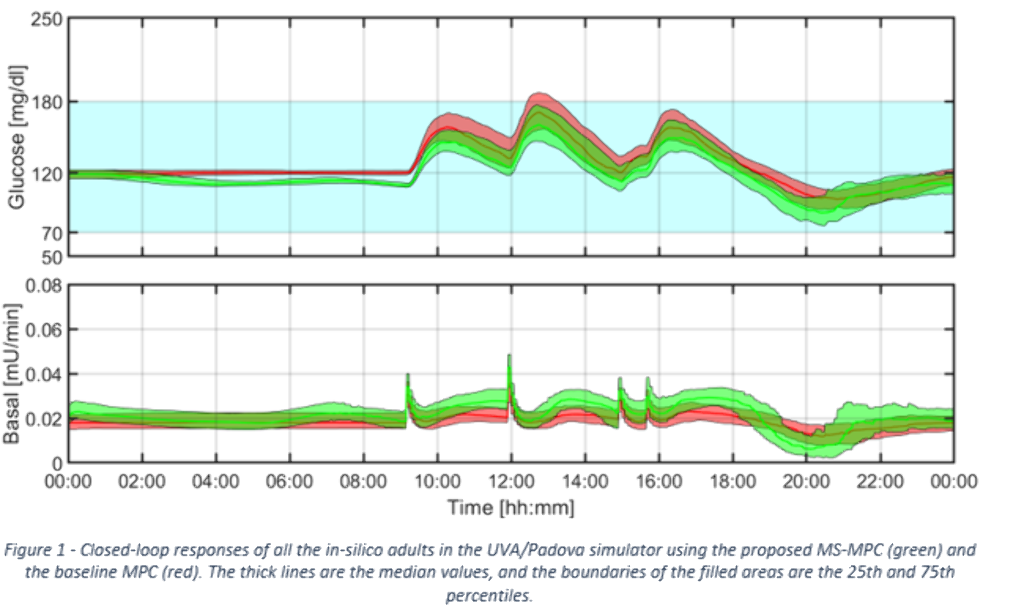
Compared to the control MPC, the MS-MPC achieved lower 3-hour postprandial mean blood glucose (BG) (139.80(±12.53) v. 146.62(±12.76) mg/dL, p <0.01), more time in the 70-140 mg/dL range (60.09% (±17.08%) v. 48.82%(±18.31%), p<0.01), greater time in the 70-180 range (90.25% (±10.88%) v. 87.86%(±12.48%), p<0.01), and less time >180 (9.74% (±10.86%) v. 12.14%(±12.48%), p<0.01). The BG standard deviation for the MS-MPC group was higher than the control group (24.71 (±8.47) v. 23.51(±8.02) mg/dL, p<0.01). There was no significant difference between percent time spent <54, <70, and >250 mg/dL.
Conclusions
These preliminary, in-silico results suggest that the use of anticipatory meal profiles can increase tight time in range and reduce mean BG for some subjects that exhibit regular eating behavior in a MS-MPC in comparison to a standard, well-tuned MPC.
CLOUDCONNECT: A WEEKLY, METRIC-INFORMED REPORT TO INCREASE FAMILY COMMUNICATION AND IMPROVE T1D MANAGEMENT
Abstract
Background and Aims
Adolescents with T1D rely on the support of their parents and the transition of responsibility during adolescence is often difficult. Only a small percentage of adolescents meet HbA1c standards. We aim to create a system that uses automated, data-driven weekly reports to improve the management of T1D for adolescents in part through improving diabetes-specific communication.
Methods
We are recruiting 40 dyads of adolescents with T1D and their parents in a 3-month randomized clinical trial. A weekly diabetes management report is generated using an algorithm that synthesizes insulin, activity, and CGM data to provide glucose management information and depict patterns of glycemic risk. The CloudConnect report also provides suggestions about diabetes management and weekly achievements. During the study, participants share CGM values in real-time with their parents. We assessed a validated score of reported diabetes-related conflict (Diabetes Family Conflict Scale, DFCS) before and after the intervention.

Results
Of the 10 dyads that have completed the study, 6 (4 male adolescents, mean age = 16.7 (±1.2 yrs.)) were randomized to use CloudConnect. Whereas family conflict typically worsens over adolescence, our data show that the participants using CloudConnect have a tendency for improvement in DFCS over the course of the study. The experimental group had an initial mean DFCS of 27.11 (±5.09) out of 57, which reduced to 26.56 (±4.36) by the end of the study.
Conclusions
CloudConnect may highlight areas of improvement for adolescents with T1D and reduce family conflict.