
Pablo Rojo (Spain)
Pediatric Infectious Diseases Specialist Hospital 12 de OctubreAuthor Of 6 Presentations
Interactive Case 1
Expert
COVID-19: Clinical outcomes of and transmissibility in the pediatric population.
THE IDENTIFICATION AND SUBSEQUENT CROSS-PLATFORM VALIDATION OF A HOST GENE EXPRESSION SIGNATURE FOR DIFFERENTIATING BETWEEN MIS-C AND OTHER INFECTIOUS AND INFLAMMATORY DISEASES
Abstract
Backgrounds:
Multisystem Inflammatory Syndrome in Children (MIS-C) occurs several weeks after SARS-CoV-2 infection with symptoms including fever, shock and multiorgan failure. Clinical features of MIS-C overlap with Kawasaki Disease (KD), bacterial, and viral infections, making accurate diagnosis challenging. Host genes, measurable through whole blood transcriptomics, are an alternative tool for diagnosing infectious and inflammatory diseases.
Methods
Patients with MIS-C, KD, bacterial, and viral infections were recruited to the EU-funded PERFORM and DIAMONDS studies and the NIH-funded PREVAIL study. Patients were phenotyped using a standardised algorithm. Genome wide RNA sequencing of whole blood was undertaken, and feature selection was performed to identify a diagnostic signature for distinguishing between MIS-C and other infectious and inflammatory conditions. The expression levels of the genes identified were measured using RT-qPCR assays in an independent validation cohort.
Results:
Through feature selection and differential expression analysis, 11 genes with diagnostic potential were identified and taken forward into cross-platform validation using RT-qPCR. With up to 11 genes, it was possible to distinguish between MIS-C vs. KD, bacterial, and viral infections with high accuracy, with an AUC of 92.9% (95% CI: 88.2%-97.6%) in the validation cohort. The diagnostic gene signature retained its high performance when tested within the groups separately in the validation cohort: MIS-C vs. bacterial infections (AUC: 94.6%), vs. viral infections (AUC: 93.1%), and vs. KD (AUC: 89.8%).
Conclusions/Learning Points:
Despite the clinical similarities between MIS-C and other infectious and inflammatory conditions, there are key differences in gene expression profiles that can be used in diagnostic contexts. It will be necessary for the genes reported here to undergo further validation prior to their development into tests with clinical utility.
IMPACT IN ANTIBIOTIC USE AFTER IMPLEMENTATION OF AN ANTIMICROBIAL STEWARDSHIP PROGRAM AND A JOINT PROTOCOL WITH ELECTRONIC PRESCRIPTION FOR APPENDICITIS/PERITONITIS IN PEDIATRICS
Abstract
Backgrounds:
Initial antibiotic treatment in appendicitis/peritonitis significantly reduces wound infection and intra-abdominal abscess formation in patients with gangrenous or perforated appendicitis. Randomized controlled trials have shown that the use of lower-spectrum antibiotic combinations is as effective in preventing abscesses or surgical wound infections as broad-spectrum regimens.
Methods
Observational, retrospective study of patients <16 years of age admitted for appendicitis and/or peritonitis from Jan/2014 to Dec/2019 in a tertiary university hospital in Madrid, Spain. Three study periods were established: P1 2014-2015 (before Antimicrobial Stewardship Programme (ASP)), P2 2016-2018 (ASP implemented) and P3 Jan/2019-Dec/2019 (ASP and implementation of an appendicitis/peritonitis protocol with electronic prescription, including lower-spectrum antibiotic combinations and selected and clinically guided use after surgery). Antimicrobial use was analysed with the days of therapy/1000 admissions days (DOT/1000) and start of treatment/1000 hospital admissions (SOT/1000).
Results:
During the study period a total of 1619 patients met inclusion criteria. The proportion of patients without antibiotic therapy after surgery during P1, P2 and P3 was 5.6%, 3.7%, and 38.6% respectively. [C1] The evolution of antibiotic use expressed by DOT / 1000 is shown in Figure 1. SOT/1000 of ampicillin, gentamicin and metronidazole rose from 162, 190 and 190 in 2014 to 386, 402 and 409 in 2019. DOT/1000 of meropenem drop to 64.85 in 2014 to 0 in 2019.

Conclusions/Learning Points:
The implementation of an ASP and a low-spectrum antibiotic protocol with electronic prescribing, reduced the antimicrobial use in children with appendicitis/peritonitis. The proportion of patients without antibiotic therapy after surgery increased and the use of carbapenems and other broad-spectrum antibiotics was reduced after the intervention. These improvements were observed when an electronically available protocol was added to the ASP implementation.
DESIGN AND IMPLEMENTATION OF A BREATH-RATE MEASUREMENT SOLUTION BASED ON COMPUTER VISION AND MACHINE LEARNING TECHNIQUES IN CHILDREN WITH LOWER RESPIRATORY INFECTION
Abstract
Backgrounds:
Camera-based diagnostic methods could allow an objective analysis of a patient's health remotely and contactless, which is especially interesting in telemedicine and pandemic scenarios. Artificial intelligence and computer vision can provide the diagnostic tools needed to improve patient monitoring. The main objective of this work is the design and implementation of a solution to estimate respiratory rate (RR) from a video captured through a smartphone, based on computer vision and deep learning techniques.
Methods
Prospective study of clinical information and a video of the patients’ chest with and without respiratory distress under 10 years old from November 2020 to May 2021 attending for a lower respiratory infection in a tertiary hospital in Spain. Video pre-processing was carried out using computer vision methods. As an initial approximation, remote photoplethysmographic signal (rPPG) was used with subsequent processing using the Discrete Wavelet Transform (DWT) and different methods to estimate the RR.
Results:
19 patients were included and 22 video sequences were pre-processed to carry out the estimation of the respiratory rate using the PPG signal approach. 51.3% were males and the average rate age was 2 years (DE 0.32). 61.5% patients had not relevant medical records. 48.7% were diagnosed of bronchiolitis followed by 30.1% diagnosed of asthma symptoms. Results obtained by different methods to estimate the RR can be seen in Table 1.
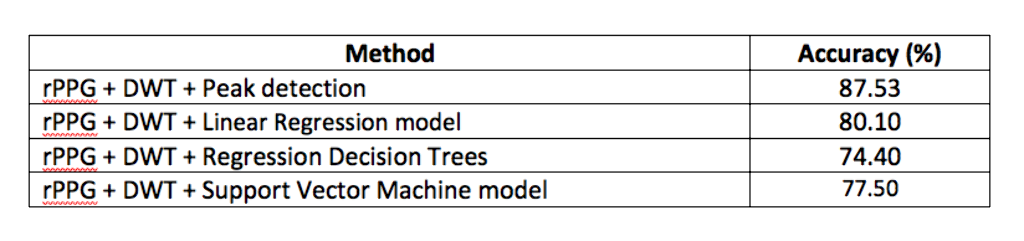
Conclusions/Learning Points:
It has been possible to design a breath-rate measurement solution to estimate RR from a video, based on DWT transformation to rPPG signal. This could be the first step in order to implement a breath-rate measurement solution based on computer vision and deep learning techniques.
Presenter of 3 Presentations
COVID-19: Clinical outcomes of and transmissibility in the pediatric population.
Interactive Case 1
Expert
Moderator of 1 Session
Poster Author Of 4 e-Posters
EP338 - CONCORDANCE ON RESPIRATORY RATE EVALUATED THROUGH A VIDEO RECORDING IN CHILDREN WITH LOWER RESPIRATORY INFECTION (ID 1177)
EP484 - PAPILLEDEMA IN PATIENTS WITH MULTISYSTEM INFLAMMATORY SYNDROME: IS AN OPHTALMOLOGICAL EXAM USEFUL? (ID 360)
- Alberto Muñoz (Spain)
- Ana Ortueta (Spain)
- Cristina Lopez (Spain)
- Sara Domínguez (Spain)
- Elisa Fernandez (Spain)
- Cinta Moraleda (Spain)
- Daniel Blázquez-Gamero (Spain)
- Luis Prieto (Spain)
- Jaime Carrasco (Spain)
- Angela Manzanares (Spain)
- David Torres (Spain)
- Serena Villaverde (Spain)
- Pablo Rojo (Spain)
- Cristina Epalza (Spain)
PD091 - CLINICAL IMPACT AFTER IMPLEMENTATION OF AN ANTIMICROBIAL STEWARDSHIP PROGRAM AND A JOINT ELECTRONIC PROTOCOL FOR THE MANAGEMENT OF PATIENTS WITH APPENDICITIS AND/OR PERITONITIS IN PEDIATRICS (ID 775)
- Serena Villaverde (Spain)
- Patricia Brañas (Spain)
- José Manuel Caro (Spain)
- Rocío Morante (Spain)
- Irene Gómez (Spain)
- Gloria Mirete (Spain)
- Cinta Moraleda (Spain)
- Daniel Blázquez-Gamero (Spain)
- Angela Manzanares (Spain)
- David Torres (Spain)
- Elisa Fernandez (Spain)
- Luis Prieto (Spain)
- Pablo Rojo (Spain)
- Cristina Epalza (Spain)
PD113 - LONG TERM ESTHETIC AND FUNCTIONAL OUTCOMES IN CHILDREN WITH NONTUBERCULOUS MYCOBACTERIAL LYMPHADENITIS (ID 1289)
- Angela Manzanares (Spain)
- Marta Nabal (Spain)
- María Collada (Spain)
- Carmen González (Spain)
- Estrella Esquivel (Spain)
- María Dolores Delgado (Spain)
- Eunate Martí (Spain)
- Jesús Redondo (Spain)
- Paula López-Roa (Spain)
- Nuria Alberti (Spain)
- Elisa Fernandez-Cooke (Spain)
- Luis Prieto (Spain)
- Cinta Moraleda (Spain)
- Cristina Epalza (Spain)
- Serena Villaverde (Spain)
- Pablo Rojo (Spain)
- Daniel Blázquez-Gamero (Spain)




