Pilar Isabel Beato víbora, Spain
Badajoz University Hospital Endocrinology and NutritionPresenter of 2 Presentations
AUTOMODE EXITS IN COMMERCIALIZED HYBRID CLOSED-LOOP SYSTEM
Abstract
Background and Aims
Hybrid closed-loop systems automatically deliver insulin based on sensor data. MiniMed 670G system operates in Auto Mode but exits to Manual Mode for certain reasons. The aim was to evaluate the duration, frequency and main reasons for exit from Auto Mode to Manual Mode.
Methods
Patients with type 1 diabetes using hybrid closed-loop system (Medtronic MiniMed 670G) for 3 months were evaluated. 2-week downloads were analysed to assess all the Auto Mode exits during this period of time.
Results
Data from 58 patients were included, age: 28 ± 15 years (7-63), 59% (n=34) females, diabetes duration: 15 ± 9 years, HbA1c: 7.0 ± 0.6%, TIR (70-180 mg/dl): 73 ± 9%.
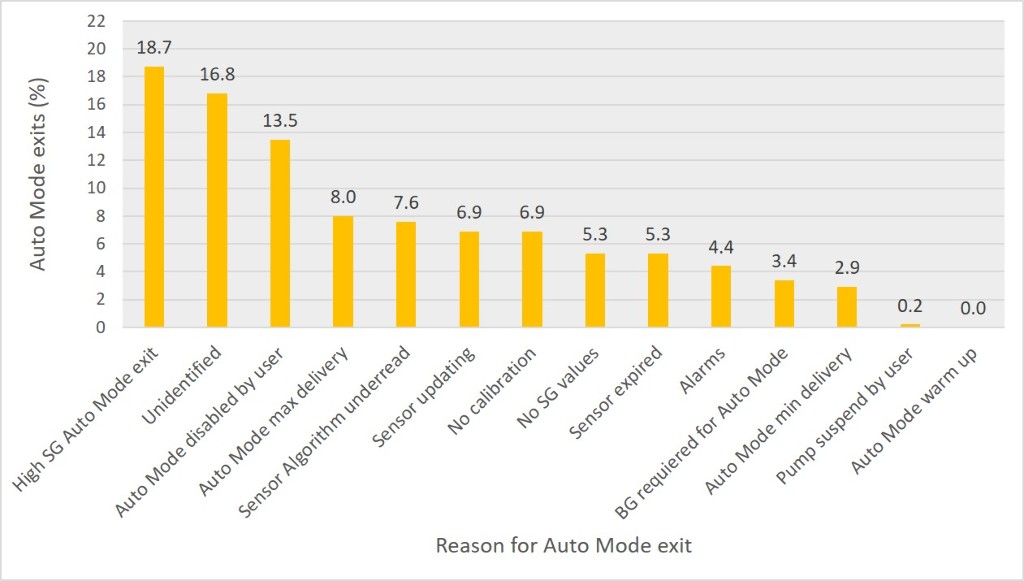
Sensor use was 86 ± 13%. Time in Auto Mode was 85 ± 17%. Number of exits was 4 ± 2 per week (0.6 ± 0.3 per day). 16.8% of the exits were not explained. Sensor issues caused the majority of explained exits (39%), followed by hyperglycaemia (23%), auto mode disabled by user (16%) and maximum or minimum insulin delivery (13%). Frequency of exit reasons is shown in Figure 1.
Conclusions
MiniMed 670G hybrid closed loop is maintained in Auto Mode during a high percentage of the time. The main reasons for exit to Manual Mode are sensor related, followed by high sensor glucose. A high percentage of exits are not explained. Time in Auto Mode should be maximized to improve the efficacy of the system and to avoid the burden of frequent interaction with the system for people with type 1 diabetes.
PROSPECTIVE EVALUATION OF THE IMPACT OF HYBRID CLOSED-LOOP SYSTEM ON GLYCAEMIC CONTROL, GLYCAEMIC VARIABILITY AND PATIENT-RELATED OUTCOMES IN CHILDREN AND ADULTS IN SPAIN
Abstract
Background and Aims
The aim was to evaluate the outcomes of hybrid closed-loop system in children and adults with type 1 diabetes.
Methods
Patients consecutively starting hybrid closed-loop system (MiniMed-670G) were evaluated in a prospective longitudinal design (baseline, 3-months, 6-months). HbA1c, time in range (TIR) 70-180mg/dl, time >180mg/dl, >250mg/dl, <70mg/dl and <54mg/dl in 2-week downloads were recorded. Glycaemic variability measures were calculated. Adolescents and adults completed a set of questionnaires (Gold and Clarke scores, Hypoglycemia Fear Survey [HFS], Diabetes Quality of Life [DQoL], Diabetes Treatment Satisfaction [DTS], Diabetes Distress Scale [DDS], Pittsburgh Sleep Quality Index [PSQI]).
Results
58 patients were included, age: 28±15 years (7-63), <18 years-old: 38% (n=22), 59% (n=34) females, diabetes duration: 15±9 years, previous treatment: sensor-augmented pump with predictive low glucose suspend (SAP-PLGS): 60% (n=35) (median time: 3.2 years [1.7-3.7]), pump+SMBG: 19% (n=11), MDI+SMBG: 12% (n=7), MDI+CGM: 9% (n=5).

At 3 months, number of auto-mode exits: 4±2/patient-week (0.6±0.3/patient-day), time in auto-mode: 85±17%, alarms: 8.5±3.7/day. Improvement in TIR was not different in children compared to adults, previous pump or CGM users compared to non-users. Baseline HbA1c and baseline TIR were predictors of improvement in TIR. In patients with baseline high hypoglycaemia risk (n=29), time in hypoglycaemia range was significantly reduced. At 6 months (n=21), HbA1c and TIR 70-180 mg/dl improved compared to baseline (HbA1c: 6.9±0.4% vs 7.3±0.7%, p=0.003, TIR: 73±8% vs 64±11%, p<0.001). Discontinuation rate was 3% (n=2).
Conclusions
Real-world use of hybrid closed-loop systems improves glycaemic control, reduces glycaemic variability and ameliorates diabetes burden in children and adults with type 1 diabetes.